Your questions about the management of the coronavirus outbreak answered
By MPs on the House of Commons Health and Social Care Select Committee
Your questions answered
In advance of our session on preparations for coronavirus (Covid-19) held on Thursday 26 March, we asked you which questions you had for the experts we had invited that day.
Tomorrow in our first session the Select Committee will be hearing from Yvonne Doyle, Medical Director Public Health England, Chaand Nagpaul of the BMA, Katherine Henderson of the Royal College of Emergency Medicine and possibly others. Any questions you would like asked to them?
— Health and Social Care Committee (@CommonsHealth) March 23, 2020
The first part of our meeting was dedicated to the impact of coronavirus on the health sector. We spoke to:
- the Medical Director at Public Health England
- the Chair of the British Medical Association
- the President of the Royal College of Emergency Medicine and
- a doctor from Northwick Park Hospital.
For the second part, we spoke to those involved in the social care sector on current preparedness for the epidemic in care homes and care services:
- The Association of Directors of Adult Social Services (ADASS)
- The Local Government Association (LGA)
- Care England
- The Care and Support Alliance
You wanted to know about testing

Can we see the policy about testing and contact tracing?
— Sallie Roderick (@salliebacon) March 23, 2020
How are the government and experts using lessons learned from China, S Korea to inform UK policy?
Why are we not following WHO guidelines on testing, contact tracing and isolation?
— paul roderick (@paulrsoton) March 23, 2020
Chair Jeremy Hunt asked:
"Countries that had an outbreak much worse than ours, such as South Korea, did not stop the testing and contact tracing. So why is our strategy different?"

Professor Doyle, representing Public Health England, gave us this explanation:
"What was different about South Korea was that these were clusters of cases where the initial transmission was well understood, because they were in particular communities and actually it was quite regional. South Korea also did something that we have looked at carefully, which is that they used technology to contact trace. They were using people’s personal details, including their bank accounts.
We have looked at that, and SAGE looked at it and felt that it was not appropriate here. However, we are still looking at applications that might be able to give us some information about conveying between people precautionary information.
The other element of breaking transmission isn’t just contact tracing and isn’t contact tracing in this phase; it is about social distancing and shielding. All countries are involved with this, but we have particularly, as you know, taken that as an effective way of breaking transmission, which is the issue about contacts."
You wanted to know about antibody tests

Please tell us all you can about the antibody tests - when will they be here? how will the testing be managed? Who will be tested?
— James Wilson (@JWilsonsGhost) March 23, 2020
Committee member Sarah Owen asked:

"If you have caught the COVID-19 coronavirus and you test positive for the antibodies, what evidence do we have that that actually provides immunity, and how long will that immunity last for? If we don’t know, what purpose are these antibody tests actually providing? "
This is what Professor Doyle, representing Public Health England, replied:
"On what antibody testing tells us, it will tell us two things. It will tell us who is highly unlikely to transmit infection, which is important because it allows people to get back to some form of normality, including work.
It also tells us about what is going on in the population, in terms of zero prevalence. That is not the sole purpose of doing antibody testing, but a proportion of the testing will look at what is going on in the population so that we understand much better what this epidemic is doing."
You wanted to know about Personal Protective Equipment (PPE) and asymptomatic people

Please ask if they agree with PHE guidance about using PPE - ie only for confirmed or suspected Covid 19 patients and NOT for asymptomatic or pre-symptomatic possibly infected Covid patients (ALL PATIENTS)
— Doug Whitelaw (@DouglasWhitelaw) March 23, 2020
1. How can we protect against asymptomatic transmission by health care workers and care workers if they aren’t all wearing at least basic masks?
— MYS (@MYST_CRT) March 23, 2020
In light of the evidence that a high proportion of Covid-19 sufferers are asymptomatic, is the guidance to self-isolate for 14 days correct? Surely the correct isolation period is 21 days to allow any asymptomatic infection to subside as well. Thank you.
— Sunil Mehra (@SunilMKP) March 23, 2020
Chair Jeremy Hunt asked:
"You said that you could pass on the virus when you are asymptomatic, for potentially up to five days. Does that mean that, today, NHS staff are likely to be passing on the virus to their patients? "
Professor Doyle, representing Public Health England, replied:
"People tend to most infectious at the beginning of this disease, particularly if they are severely unwell, and that does tail off. That is the issue about what happens between seven and 14 days; other important things do happen between seven and 14 days with those who are hospitalised.
So, the answer in theory is yes, and at the beginning, particularly when people are symptomatic at the beginning, they may be at their most infectious, but we are still learning."
You wanted to know about plans to support social care providers

Are there any plans to support social care providers who are experiencing higher costs during this crisis, to enable them to stay sustainable and recognise the extra efforts of their staff. Care Association Alliance
— Melanie Weatherley MBE (@MelanieWeathe12) March 24, 2020
Chair Jeremy Hunt asked James Bullion, who represented ADASS:
"Could you give us your take, from the ADASS perspective, about whether that £1.6 billion will be enough?"

This is what James Bullion from ADASS replied:
"I do not think it will be enough, but it is a good start.
It is already very clear that the costs involved in providers taking on agency staff and dealing with sickness, PPE and all of that, are likely to be 30% to 40% higher than the usual rate that we would pay. We are going to have to pay our way out of trouble on this issue, and I think we might have to come back for additional funding."
Sarah Pickup, representing the LGA, added:
"We have to think about the entirety of the people who need social care, not just those who need to be discharged from hospital. We know that we need to work with providers to ensure that they can access staff for all those purposes.
It is about not just the rate but the speed of payment—payments up front, payment on plan and so on. We need to take a whole range of measures to support providers. It is absolutely vital, but it is unfortunately not simple. Guidance is coming out very rapidly. There is guidance on discharge, guidance for commissioners, and I think guidance on fees is coming shortly."
You wanted to know about hospital discharges
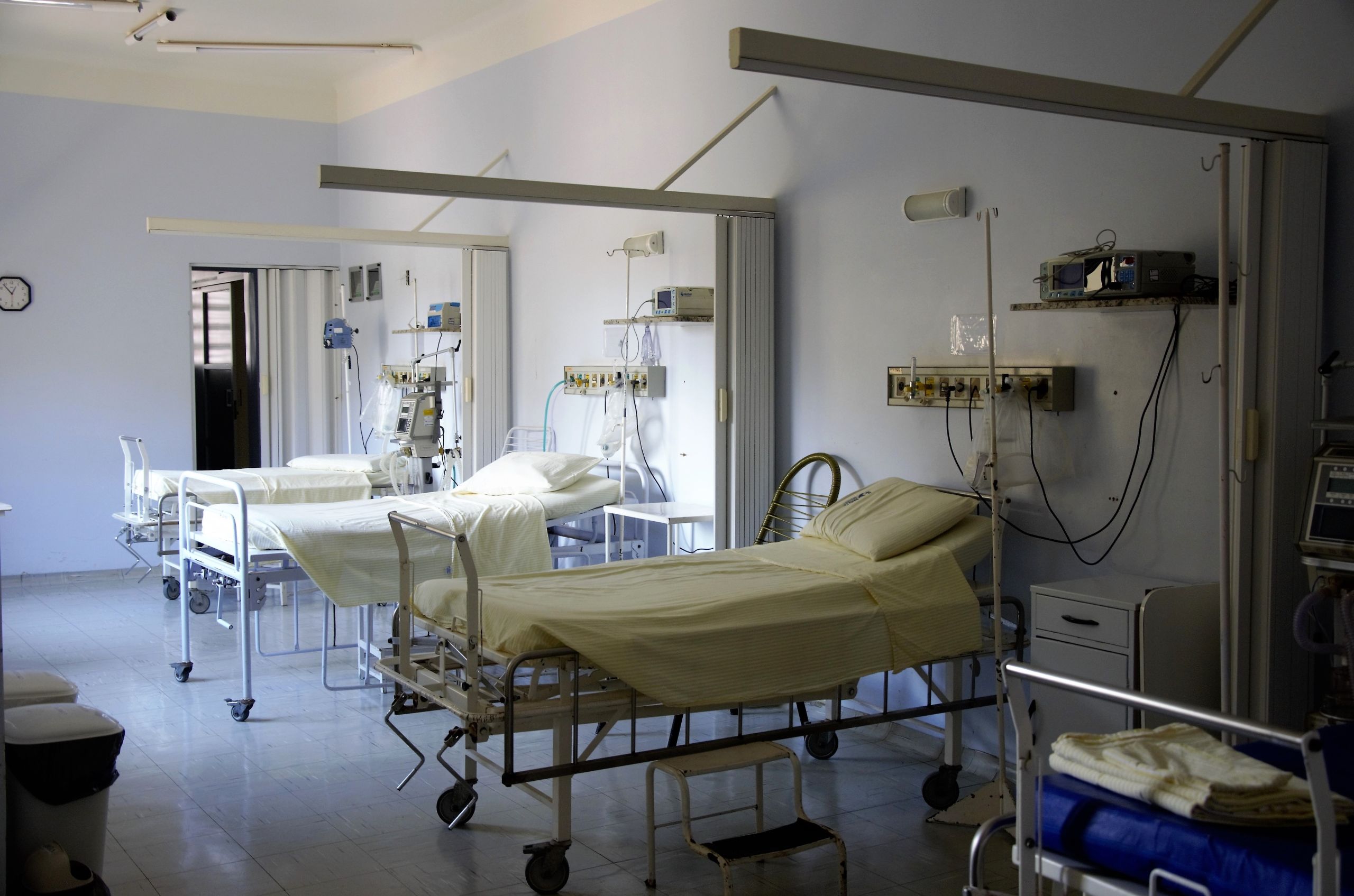
@CommonsHealth Social and Community Care urgently need good communication to be able to quickly accept hospital discharges safely. Discharge criteria and advice, ongoing care and financial arrangements
— beverley proctor (@beverleyproctor) March 23, 2020
Committee member James Murray asked:
"There was a commitment from Ministers to a target that the discharge of people from NHS hospitals into social care settings should make at least 15,000 hospital beds available by tomorrow. Do you get the sense from conversations or feedback that we are on track to get those 15,000 beds freed up, and if not, what more help do you need? "
James Bullion, representing ADASS replied:
"Yes, the discharge to assess process is very ambitious and it does talk about 15,000 beds. I can see that authorities up and down the country will be doing the maths and trying to identify where that capacity will come from. I think that the limiting factor on our success will be the PPE and the providers feeling assured that they can take people either into care homes or back home for home care. That is the first limiting factor.
The second, though, will be the workforce and plugging the gap.
Thirdly, the flow arrangements within our hospitals are still not perfect. We have removed all the bureaucracy, we have removed the funding question, and we have removed some of the legislative factors requiring an assessment, a continuing healthcare assessment or a financial assessment, but we still have this flow issue about identifying the people who are safe to discharge."
You wanted us to pursue recognition of the role of social care

When will social care be recognised for the important role it plays in the health of this nation?
— Julienne Meyer CBE (@JulienneMeyer) March 23, 2020
Committee member Paul Bristow asked:

"I am interested in how we improve the morale of social care staff, because the staff who work in the social care system are at the frontline of the crisis and their morale is a key factor in ensuring the wellbeing of the people they provide for. "
Emily Holzhausen, representing the Care and Support Alliance, replied:

"Absolutely; I could not agree more. Every time someone says, “Our NHS staff are doing an amazing job,” I can hear myself saying, “And social care. And social care.” I say to all of you, who are leaders and do quite a lot of media work, that just hearing that over the airwaves and seeing it in print and online, consistently, about the NHS and social care would make such a difference."
Transcripts of our oral evidence sessions, can be found on our website.
If you’re interested in our work, you can find out more on the House of Commons Health and Social Care Select Committee website. You can also follow our work on Twitter.
The Health and Social Care Committee is a cross-party committee of MPs that scrutinises the work of the Department of Health and Social Care and its associated public bodies.
Cover image credit: PIRO4D,Pixabay.com

